Virtual behavioral health and telemedicine services are often highlighted for offering convenient, affordable, and scalable care while lowering barriers to access. But emphasis on accessibility alone has created a persistent myth: that virtual care is best suited for “simple” patients with mild symptoms, while those with more severe anxiety or depression require in person treatment to see meaningful improvement.
At Array Behavioral Care’s AtHome service model, a fully virtual behavioral health program delivering measurement-based psychiatry and therapy services to patients in their own home, our data tells a very different story.
In fact, our recent white paper, Proven at Scale: Real-World Outcomes from a Virtual Behavioral Health Model, highlights a powerful and consistent pattern: patients who enter virtual care with higher symptom severity, particularly those with baseline PHQ-9 or GAD-7 scores at or above 10, experience larger absolute gains than lower acuity patients. These findings challenge long-held assumptions about who can benefit most from digital behavioral health.
And the implications are not subtle. They suggest that virtual care may be especially well positioned to support complex, high-need individuals who historically struggle to access traditional services.
THE STEREOTYPE: Virtual care is for “easy” patients
For years, virtual therapy has been viewed primarily through the lens of access and convenience: something light, low touch, and suitable for individuals with adjustment issues or mild mood and anxiety disorders. Patients in crisis, those facing challenging social determinants of health, or those with moderate to severe disorders were generally assumed to require in person care.
This assumption is so widespread that many healthcare decision makers continue to treat virtual care as a second-tier option, useful only when face-to-face services aren’t feasible, rather than recognizing it as a best-in-class solution capable of addressing critical gaps in their fragmented care systems.
But the data we’ve collected across more than thirty thousand virtual encounters paints a different, more encouraging reality.
THE REALITY: High acuity patients improve more, not less
- Patients with PHQ-9 > 10 or GAD-7 > 10 (moderate depression or anxiety) consistently demonstrated larger absolute reductions in scores than those with mild symptoms.
- These improvements held across diverse demographics and clinical subgroups.
- The magnitude of improvement was large enough to be clinically significant, not just statistically detectable.
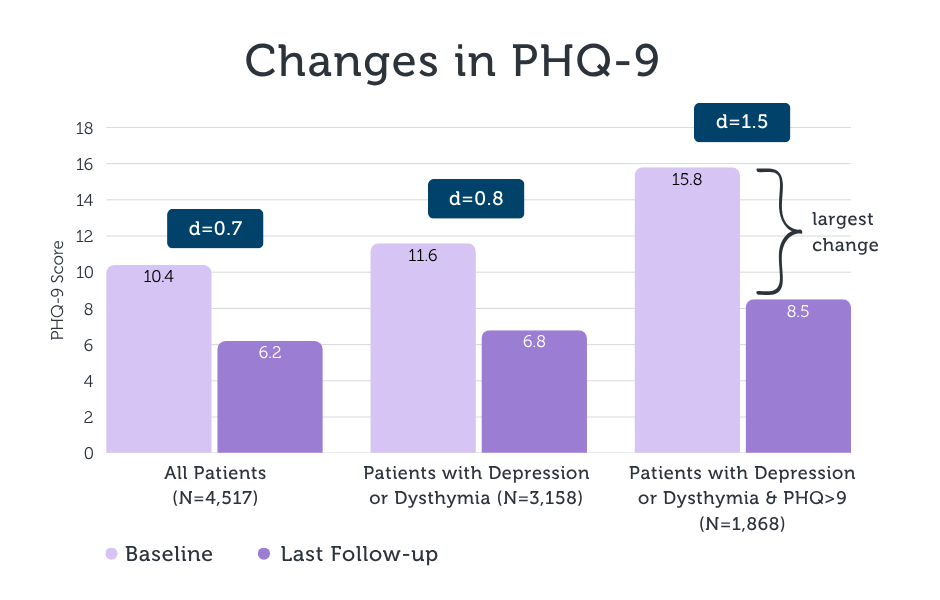
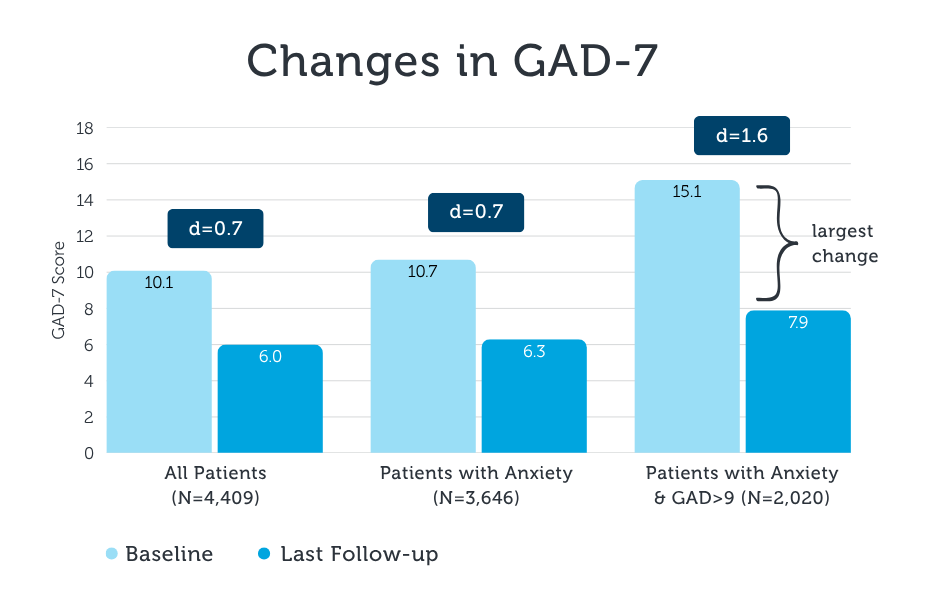
*Cohen’s d is a standardized effect size that expresses the magnitude of a difference in continuous outcomes in standard‑deviation units, with conventional benchmarks of 0.20 (small), 0.50 (medium), and 0.80 (large).
Instead of plateauing or showing diminished gains, high acuity patients responded robustly, and in some cases quite dramatically, to virtual interventions. In fact, the magnitude of their improvement, reflected in effect sizes of d = 1.5 (depression) and d=1.6 (anxiety), fall in the “very large” range. In simple terms, an effect size is a way of measuring how big the change really is: while small effects indicate modest shifts, a very large effect size means the average patient improved far more than would typically be expected in behavioral health treatment.
This finding flips the old narrative. Virtual care isn’t merely “good enough” for high acuity patients, it may be an optimal environment for treating them.
Why higher acuity patients may thrive in virtual care
1Faster access → Faster relief
2Reduced overwhelm and stigma
3Tailored interventions delivered at scale
A new understanding of virtual care’s role in complex populations
The data Array has collected and reported in our recent white paper, Proven at Scale: Real-World Outcomes from a Virtual Behavioral Health Model, suggests that virtual behavioral health care should not be seen as a preferable starting point only for lower acuity cases. Instead:
Virtual care may be uniquely suited for individuals with moderate to severe mental health symptoms.
This reframes virtual services not as the “lightweight” alternative, but as a high value, high impact option for complex patients that have historically been underserved and at greatest risk for poor outcomes.
Implications for health systems and payers
If virtual care delivers the biggest absolute gains for high acuity patients, several strategic implications follow:
Prioritize high severity intake through virtual channels
Rapid engagement can accelerate improvement and prevent symptom escalation.
Shift utilization assumptions
Reevaluate cost assumptions
Integrate virtual care as a core, not peripheral, part of behavioral health strategy
Conclusion: Virtual care’s sweet spot is high acuity, not low acuity
Contrary to longstanding stereotypes, our rigorously collected data shows that virtual care doesn’t merely work for high acuity patients; it often works best for them.
Patients with baseline PHQ-9 or GAD-7 scores at or above 10 experienced larger overall improvements than those with milder symptoms, demonstrating virtual care’s capacity to deliver meaningful, measurable change in some of the most challenging clinical scenarios.
In other words:
High acuity isn’t a barrier for virtual care; instead it’s where virtual care shines brightest.
References
1 Tran Q. D. (2024). Going Beyond Waitlists in Mental Healthcare. Community mental health journal, 60(4), 629–634. https://doi.org/10.1007/s10597-024-01233-2
2 Ahmedani, B. K., Yeh, H. H., Penfold, R. B., Simon, G. E., Miller-Matero, L. R., Akinyemi, E., Fallone, M., Patel, S., Beebani, G., Hooker, S. A., Owen-Smith, A., Knowlton, G., Levin, A., Eke-Usim, A., & Rossom, R. C. (2024). Psychotherapy Disruption Before and After the Transition to Virtual Mental Health Care Induced by the COVID-19 Pandemic. Psychiatric services (Washington, D.C.), 75(2), 108–114. https://doi.org/10.1176/appi.ps.20230181
3 U.S. Department of Health and Human Services. (n.d.). Telehealth for behavioral health care. Telehealth.HHS.gov. https://telehealth.hhs.gov/providers/best-practice-guides/telehealth-for-behavioral-health
4 Luo, C., Sanger, N., Singhal, N., Pattrick, K., Shams, I., Shahid, H., et al. (2020). A comparison of electronically delivered and face to face cognitive behavioral therapies in depressive disorders: A systematic review and meta analysis. eClinical Medicine, 24, 100442. https://doi.org/10.1016/j.eclinm.2020.100442

